I received this short email after I posted my blog on stories of surgical despair.
Hi David,
I’m grateful you’re collecting these stories. My dad passed away on January 27 due to his last cervical fusion. It’s tragic, and I’m devastated. I asked him to reconsider before the surgery last August, but of course, the surgeon convinced my dad it was necessary. He regretted it almost immediately because he could never swallow normally again and ultimately lost his fight after months in the hospital and rehab. Thank you for your efforts to raise awareness — I truly hope it helps change the spine surgery industry. I’m forever thankful for you.
❤️ Dana
Two failed spine surgeries
Dana was a young woman I met about five years ago after she discovered the Curable app and came across one of my interviews. She reached out and soon joined my course and weekly coaching group as she was working to recover from chronic pain following two unsuccessful spine surgeries. Her original symptoms involved her lower extremities, particularly significant calf and sciatic pain. Initially, she didn’t have much back pain. However, during a second surgery to repair a tear in her dura, complications arose, leading to further damage to her spinal column and nervous system. After that procedure, her pain became widespread and severe, affecting her entire body.
At her worst, she could barely get out of bed, and her partner was incredibly supportive throughout that time. By the time we connected more regularly, she was able to function better but still dealt with significant pain and emotional distress.
She had already tried many approaches and was very informed. She engaged deeply in the work, participating in both the course and the group. While she made progress, she continued to experience more pain and limitations than she wanted. To be honest, I wasn’t sure how much further she could go. At one point, I told her, “Stop.” Stop searching for more answers and begin leaning into the life you want to live, with or without the pain.
Her healing journey
Within about six weeks, she experienced a significant change, with her pain decreasing by approximately 80%. Over time, she became essentially pain-free and without functional limitations. We were all excited about her recovery, and I have to admit, I was a bit surprised.
Her partner, a documentary filmmaker, captured her healing journey in a film called “Love Heals,” which can be viewed at lovehealsfilm.com.
This may seem unusual to some, but one of the foundational books related to this concept is The Way to Love by Anthony DeMello. He defines love as awareness. This reflects a profound shift in the body’s chemistry from a state of threat, where the body breaks down, to a state of safety, where it regenerates and heals. This is a physiological shift, not a psychological one. It requires learning skills to move out of a fight-or-flight stage into one that allows healing. The skills are presented in my course, The DOC Journey, in a sequence that requires 10-20 minutes a day. Meaningful change usually occurs over three to six months. I did not heal her, nor did the course. The course is simply a framework and curriculum that presents documented, effective treatments in an accessible manner. She was the one who figured out how to heal.
There is a reason why giving up looking for yet another answer is central to healing. Endlessly seardhing for a solution keeps your attention on the pain. Healing occurs as you reprogram your nervous system away from pain circuits, and focus on living life on your terms. Your brain changes every second and you’ll develop new circuits without the pain. However, you also have to learn to let go in order to move forward. She had done a lot of work in learning to let go, and her healing was dramatic as she moved forward. Dana’s story is inspiring, and I encourage you to watch the film.
Her father’s tragedy
Never underestimate the potential impact of an invasive procedure on your life. Even the simplest procedures can have devastating consequences. If a complication were planned, it would not be a complication. Cervical spine surgery is delicate and carries significant risks. Even after a perfectly performed operation, swallowing issues are not uncommon. Usually, they resolve over three to four months, but some are permanent, and his turned out to be catastrophic. I don’t know if he needed the surgery or not, but it is critical to prepare yourself with a prehab program. Often, surgery is avoided.
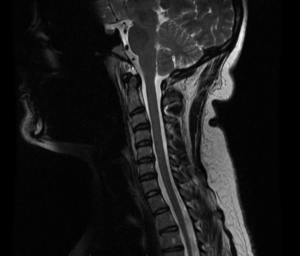
Patients may be convinced that they need surgery even though their symptoms are not that bad. I would never decide whether a patient should have surgery, except for an emergency. Patients would become frustrated because I would not give them a concrete answer. But I pointed out that “I am not you, I don’t know the level of your discomfort, and how well you are tolerating your symptoms.” Any recommendation would be based on my interpretation (projection) of what they were saying. It was important that they understood the nature and magnitude of the operation, so they could make the final decision of the risks versus the benefits. Many patients simply decided to live with their symptoms. Eventually, I realized that many patients were suffering more from mental pain than physical pain. This realization had a dramatic impact on my surgical decision-making, and I had every patient considering elective surgery undergo a prehab program.
There are no shortcuts
The most disturbing part of both of these stories for me is knowing what’s possible versus what often happens. Patients frequently choose a quicker fix. They see the healing journey as too much work and just want to finish it quickly. It’s not entirely their fault because medicine is based on an inaccurate model. There is extensive data on the physiological roots of chronic illness, symptoms, and disease. I’m not sure why mainstream medicine remains so disconnected from this research.
I quit my practice the day I ran across a young gentleman who was paralyzed by a surgery on a stable spine that he did not need. The contrast between watching 3-5 patients a week experiencing ongoing problems created by spine surgery and watching so many patients experience deep healing with minimal resources became intolerable. Do not undergo any surgery or any procedure without understanding all aspects of it and preparing yourself. Take control of your care and decision-making. Don’t become a statistic. Get it right the first time.
