Video animation of a lumbar fusion
The purpose of this letter is to explain what is involved when a posterior fusion is performed on your lower back. We have found that the more knowledgeable the patient, the more successful the surgical outcome. Patients undergoing this procedure most commonly ask the following questions.
What is a lumbar fusion?
A lumbar fusion is a procedure in which two or more vertebrae in the low back are “welded” together to create a solid bridge of bone between the vertebrae and across the disc space. A fusion is usually performed to eliminate movement between vertebrae and stabilize a painful or unstable segment of the spine. Once a segment of the spine is stabilized the patient usually experiences some relief of pain. Surgery is not recommended unless there is a 70% chance or better of improving your level of pain. This improvement does not necessarily mean that you will be completely pain free but rather that your level of pain should be significantly improved. It means that there is a some chance your pain will not improve. However, each situation is unique. There is also at least a small chance that you may become significantly worse.
Will I lose mobility once a portion of my spine becomes solid bone?
It depends in part on how much of the spine is fused. The spine will not move as much but you may not notice it, as it is only a small amount. Most people believe that the spine enables you to bend over at the waist; this motion actually occurs mostly at the hips. There are patients that have their entire spine fused yet are still able to touch their fingertips to the floor.
What happens during a lumbar fusion?
At the hospital you are given a general anesthetic to put you to sleep. Once you are asleep, padding is placed between your body and the table and you are carefully positioned face down. An incision is made over your lower back and your muscles are gently pulled away from your spine to expose the lumbar vertebrae. If your nerves are under any pressure they are decompressed via laminectomy, laminotomy or foraminotomy. Once the nerve work is completed the surgeon begins the grafting process. This may entail removing small pieces of bone from the outside part of the back of your pelvis, obtaining cadervic bone or, using bone graft extenders. The bone graft material is used to stimulate the fusion. The bone on the exposed part of your spine is then roughened up. This enables the bone to have a better surface area with which to bond. The graft is then placed closely against the roughened bony surfaces. It is this combination of bone graft material with a raw bony surface, which stimulates the bone to form a solid piece of bone. Please discuss with your surgeon the pros and cons of the different bone graft materials.
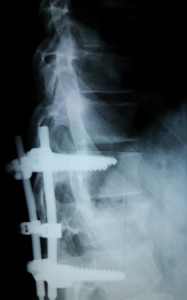
Why are screws, plates, or rods used in my spine?
Screws, plates, or rods (also known as “hardware” or spinal instrumentation) are used to immobilize the spine, this immobilization will enhance the healing process. Spinal instrumentation acts as an internal splint. Historically, braces or casts were used. However, research has found that they are not as effective in immobilizing the spine. If too much motion occurs the vertebrae may not fuse together. This is known as a pseudoarthrosis or non-union. The incidence of pseudoarthrosis ranges from 10 to 40% without spinal instrumentation. If this occurs, further surgery may be required to stimulate the bone to fuse. Screws, rods and plates have been shown to significantly decrease the rate of non-union.
Once the fusion process is completed, it is the fusion that holds the spine stable, not the spinal instrumentation. Therefore, if the fusion is solid the spinal instrumentation serves no purpose.
If the fusion is not solid, there is a high probability that the spinal instrumentation will loosen and/or break. This is not dangerous and will not cause nerve damage as the spinal instrumentation is buried deep within the fusion mass, similar to steel rods buried in concrete for reinforcement.
The benefits of the screws, rods and plates are as follows:
They help correct deformity of the spine
They give immediate stability and earlier relief of pain
They give rise to a higher fusion rate than non-instrumented fusions
Complications associated with placement of the screws include dural tears, bone breakage, nerve damage, vascular injury, and infection. Screws may also loosen or break. However, this is not typically thought of as a complication but rather as an indication that the fusion has not healed. In many cases the fusion subsequently goes on to heal without problem or need for additional surgery.
Does smoking have an effect on the outcome of my fusion?
Research shows that the healing rate is greater than 90% in non-smokers and less than 50% in smokers. Many are reluctant to perform a fusion in patients who smoke because of the higher rate of non-union, infection, and other medical complications. Physicians have also found that in smokers it is sometimes necessary to go in through the front (anterior) and the back (posterior) of your spine in order to obtain a successful fusion. If you smoke, be prepared to discuss the situation in detail with your physician.
What will my hospital stay be like?
Several nurses and doctors will ask you questions regarding your medical history. It would be helpful to bring a list of medications that you are currently using. You will wait in the holding area of the operating room for about 30 minutes before surgery. This is where you will meet your anesthesiologist and have your IV’s initiated.
After surgery you will wake up in the Recovery Area where you will remain for about two hours. There may be a catheter in your bladder. The catheter is usually removed on the 2nd or 3rd day; however, if you are unable to urinate you may need to be recatheterized. Due to the anesthesia and medications, many patients have a poor recollection of this time period.
The first 2 days will be difficult. The most painful part of recovery is often the site of the bone graft. In order to obtain an adequate amount of graft, the gluteal muscles have to be dissected. As you walk these muscles will pull on the graft site. This area will be painful until the scar matures, which may take anywhere from 4 to 6 weeks or longer and sometime permanent. As a result of these difficulties we often use a different technique or a bone graft substitute to avoid them
We will try very hard to keep you as comfortable as possible with IV narcotics. You will be able to control the amount of pain medication you receive by using a small push button. You can push the button as often as you need; the machine will control the dose. We have been very happy with the amount of pain control we can obtain with this machine.
The combination of narcotics, anesthesia, and spine surgery may cause you to experience some nausea. We allow only ice chips or small amounts of liquid until you are passing gas. If fed too soon, you may become distended and even more nauseated. About 20% of our patients are fairly nauseated within the first 24 hours. This problem is usually resolved by the third day.
We encourage you to get out of bed on the first or second day. We insist that you are ambulated as soon as possible. We have found that there is a lower incidence of lung, bladder, and vascular complications the earlier the patient is mobilized.
When can I go home and what will I be able to do?
You may go home once your pain can be controlled with pills, your incision is not draining, and your bowel and bladder are functioning normally. Most patients are ready to go home by the fourth or fifth day after surgery.
Within the first few weeks following discharge we encourage you to begin walking for one half hour to two hours each day, in divided intervals. If you were given a brace, you must wear it during the day although you can remove it to sleep or shower. You should be able to go up and down stairs, drive, and perform basic daily activities without too difficulty. You should avoid bending or twisting at the waist as that increases the stress across the fusion site. A general rule of thumb is, “nose over toes”, with respect to twisting and bending at the knee to reach objects below your waist. It usually takes a minimum of three to four months for the fusion to heal; patients who are placed in a brace require it for this entire time period. The time frame in which you can return to work depends on your recovery. Each patient has a unique set of work-related issues, which will need to be discussed with the doctor.
The first office visit should be scheduled one to three weeks after you are discharged. The purpose of this visit is to check your incision and make sure you are progressing as planned. The second visit is typically scheduled two to four months after surgery. During this visit the status of your fusion is assessed. Each physician has his own approach to rehabilitation, some more vigorous than others. Your physician will prescribe a rehabilitation program based on your specific needs.
Do I need a blood transfusion?
A spinal fusion is a major surgery, which may require a blood transfusion. If you have had prior spine surgery you will most likely need a transfusion. You can donate the blood yourself or you can use the blood bank. The blood bank is very safe; the risk of contracting AID’s is less than one in 30,000. The risk of contracting Hepatitis is one in 10,000. Most of the time the need for a blood bank transfusion can be eliminated by pre-donating your own blood. If you choose to donate your own blood you can donate from one to three pints at one-week intervals. Prior to surgery, our office will arrange the donations through the local blood bank.
What are the specific risks of this operation?
Every surgical procedure carries significant risk. These include major risks, which may have long term or negative side effects, and minor risks that do not have any long-term effects.
Major Risks
Deep Infection: 2-3%
These include infections, which may show up several months or years after surgery and require prolonged use of antibiotics. Future surgeries may also be necessary. To address this risk we place you on antibiotics during and after surgery. This lowers your risk of a postoperative infection to less than 3 or 4%.
Pulmonary Embolism: <0.5%
Occasionally a blood colt can form in your legs, break off, and travel to your lungs. Once the clot reaches the lungs they are referred to as a pulmonary embolism, which can be fatal. A pulmonary embolism occasionally occurs in spine surgery patients. If the clot is detected early it can be treated with blood thinners. To prevent blood clots from forming in your legs you will wear white support stockings as well as air pump stockings over them. This markedly decreases your chance of getting a blood clot. The risks are much higher if you have a history of blood clots. Make sure that you inform your doctor of such a history.
Pseudarthrosis: 15 – 40%
A pseudarthrosis or non-union is a term used to describe a fusion that has not healed. This means that a solid bridge of bone has not formed between the vertebrae. A non-union does not necessarily mean that the surgery must be redone; many patients with a non-union are quite happy with their pain relief. However, in cases where the pain persists, the fusion may have to be redone. We have found that smokers have a higher incidence of pseudarthrosis (>50%) than non-smokers. Therefore, you should be aware that smoking could significantly affect the outcome of your surgery.
Failure to obtain satisfactory relief 20-30%
The biggest risk of your surgery from a statistical point of view is that everything will go well, but in the end your pain will not be relieved to the degree that you had hoped. The chance of that is 20-30% for your back pain and 10-15% for your leg pain. This is just the reality of doing surgery for pain, is that it doesn’t always work. One thing you can do to help make sure you are satisfied with your results is to realize that this operation should be thought of as a pain improving procedure and not a pain eliminating procedure. It is reasonably effective at bringing pain from an unmanageable level to a more manageable level.
Dural tears: 5 – 7%
A sac of clear fluid called the dural sac surrounds the spinal cord and nerves. This sac is not routinely entered. However, if the sac is torn during surgery, it is either sewn tightly together to prevent any cerebral spinal fluid from leaking or, depending on the nature of the tear, biologically adherent compounds may be applied to the area. To heal properly you may be required to remain flat on your back for 24 to 72 hours to enable the leak to seal. If the leak persists you may require further surgery or special drains.
Nerve Damage: 1 – 2%
Nerve damage can occur due to excess traction, a screw placed too close to the nerve, or a nerve inadvertently cut during the procedure. Symptoms include numbness, weakness, and/or pain. Nerve damage is usually a temporary problem, which is isolated to only one nerve. However; it can occasionally involve multiple nerves and remain permanent. In rare instances bowel and bladder function may be lost. Paralysis is possible but very rare.
Re-operation: 15%
Further surgeries may be necessary if the spinal instrumentation breaks or loosens. Other reasons include nerve impingement form a screw, pseudarthrosis (non-healing of the fusion), infection, or persistent pain. There is about a 10% chance that the fusion may transfer stresses to the adjacent discs, resulting in degenerative disc disease and require additional surgery.
Other:
Other major complications are rare but include perforation of a major blood vessel, kidney damage, and medical complications such as heart attack, stroke and even death.
Minor Risk
Complications which are less serious include bladder infection, superficial would drainage, inability to urinate for a few days, nausea, headaches, constipation, abdominal bloating, sore throat, pneumonia, and reactions to medications. If your body is unable to replenish its blood supply or if too much blood is lost during surgery, a blood transfusion may be necessary. As with any surgery, there are also unanticipated major and minor risks.
What is your overall philosophy regarding spinal fusion?
Lumbar fusion is generally an elective surgery. Therefore, it is your choice to proceed based on your current level of discomfort and disability. We recommend that you do not have surgery if you can live with your current level of pain or can make changes in your lifestyle to decrease the pain. If you have made a valiant effort and the pain still persists, surgery should be your next step.
The rate of surgical success varies greatly depending on your exact problem, overall health, and the magnitude of surgery necessary. We hope that by providing you with as much information as possible about the surgery, you can determine if the pain you are experiencing is worth the risk of surgery.
